Depression is a mood disorder that causes a persistent feeling of sadness and loss of interest.
Not only are people with some of the major neurologic conditions more likely to develop depression, but a history of depression is associated with a higher risk of developing several of the neurologic conditions, such as epilepsy, migraine, stroke, Parkinson’s disease, and dementia.
Symptoms of Depression:
Although depression may occur only once during your life, people typically have multiple episodes. During these episodes, symptoms occur most of the day, nearly every day, and may include:
- Irritability, or frustration, even over small matters
- Anxiety or restlessness
- Feelings of sadness, tearfulness, emptiness or hopelessness
- Sleep disturbances
- Tiredness and lack of energy, so even small tasks take extra effort
- Loss of interest in most or all normal activities, hobbies, or sports
- Slowed thinking, speaking, or body movements
- Feelings of worthlessness or guilt, fixating on past failures or self-blame
- Frequent or recurrent suicidal thoughts
- Physical problems, such as back pain or headaches
- Reduced appetite and weight loss or increased cravings for food and weight gain
- Trouble thinking, concentrating, and remembering things

Specific conditions that are triggered by depression and its consequences
More than just a bout of the blues, depression isn’t a weakness and you can’t simply “snap out” of it. Depression may require long-term treatment. But don’t get discouraged. Most people with depression feel better with medication, psychotherapy, or both.
Conditions triggered are…
- Migraine:
Migraine and depression have a bidirectional relationship, meaning depression increases the risk of migraine and vice versa. Those with depression are 3.4 times more likely to develop migraine. Conversely, those with migraine are 5.8 times more likely to develop depression.
- Alzheimer’s Disease:
Depression is very common among people who have Alzheimer’s or dementia. Many times, they become depressed when they realise that their memory and ability to function are getting worse. Together, depression and Alzheimer’s dementia can cause other symptoms too. People suffering from this condition may not want to go places or see people anymore
- Stroke
A multinational study has found that people with depression symptoms are more likely to experience a stroke, and their recovery from stroke is often more difficult. Many individuals develop depression, anxiety, and other psychological sequelae. These disorders can significantly affect their lives and their relationships.
- Parkinson’s Disease
Depression is a part of Parkinson’s itself, resulting from PD-related changes in brain chemistry. Parkinson’s impacts areas of the brain that produce dopamine, norepinephrine, and serotonin — chemicals involved in regulating mood, energy, motivation, appetite, and sleep.
- Epilepsy
A person with depression has an increased risk of epilepsy. Depression and epilepsy are two different health conditions that may occur together. This may be due to neurological changes, hormones, and specific medications. Living with depression or epilepsy can significantly affect a person’s daily life
- Traumatic Brain Injury
Depression is a common problem after Traumatic Brain Injury (TBI). About half of all people with TBI are affected by depression within the first year after injury. Even more – nearly two-thirds are affected within seven years after injury.
More than half of the people with TBI who are depressed also have significant anxiety.
- Multiple Sclerosis
Long-term physical symptoms of multiple sclerosis can bring on changes in one’s mood. But Multiple Sclerosis (MS) itself might also cause depression. The disease may destroy the protective coating around nerves that helps the brain send signals that affect mood.
Depression has a significant impact on the daily function of MS patients, including their interpersonal relationships, cognition, and fatigue.

Consequences of Depression:
Untreated depression increases the chance of risky behaviours such as drug or alcohol addiction. It also can ruin relationships, cause problems at work, and make it difficult to overcome serious illnesses. Clinical depression, also known as major depression, is an illness that involves the body, mood, and thoughts.
Treatment for Depression:
The cornerstone of treatment is usually medication, talk therapy, or a combination. Increasingly, research suggests that these treatments may normalise brain changes associated with depression.
Depression is one of the most treatable mental health conditions. Approximately 80% to 90% of people with depression who seek treatment eventually respond well to treatment.
Treatment options include…
Psychotherapy:
Psychotherapy or talk therapy, involves talking with a mental health professional. The therapist helps the patient identify and change unhealthy emotions, thoughts, and behaviours. There are many types of psychotherapy — cognitive behavioural therapy (CBT) is the most common. Sometimes, brief therapy is all you need. Other people continue therapy for several months or years.
Medication:
Prescription medicine called antidepressants can help change the brain chemistry that causes depression. There are several different types of antidepressants, and it may take time to figure out the one that’s best for you. Some antidepressants have side effects, which often improve with time. If they don’t, talk to your healthcare provider. A different medication may work better for you.

Complementary medicine:
This involves treatments you may receive along with traditional Western medicine. People with mild depression or ongoing symptoms can improve their well-being with therapies such as acupuncture, massage, hypnosis, and biofeedback.
Brain stimulation therapy:
Brain stimulation therapy can help people who have severe depression or depression with psychosis. Types of brain stimulation therapy include electroconvulsive therapy (ECT), transcranial magnetic stimulation (TMS), and Vagus nerve stimulation (VNS).
There are other things one can do at home to help improve depression symptoms, including getting regular exercise and quality sleep (not too little or too much). Eating a healthy diet. Avoiding alcohol, which is a depressant. Spending time with people you care about.
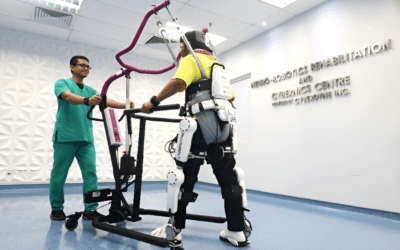
Neurological Neurorehabilitation:
Neurological rehab can often improve function, reduce symptoms, and improve the patient’s well-being.
A neurological rehab programme is designed to meet individual needs, depending on a specific problem or disease. Active involvement of the family is vital to the success of the programme.
The goal of neurological rehab is to help the patient return to the highest level of function and independence possible while improving their overall quality of life.
Neurorehabilitation programmes include:
- Help with activities of daily living, such as eating, dressing, bathing, handwriting, cooking, and basic housekeeping
- Speech therapy to help with speaking, reading, writing, or swallowing
- Stress, anxiety, and depression management
- Bladder and bowel retraining
- Activities to improve mobility (movement), muscle control, gait (walking), and balance
- Exercise programmes to improve movement, prevent or decrease weakness caused by lack of use, manage spasticity and pain, and maintain range of motion
- Social and behavioural skills retraining
- Nutritional counselling
- Involvement in community support groups
- Activities to improve cognitive impairments, such as problems with concentration, attention, memory, and poor judgement
- Help with obtaining assistive devices that promote independence
- Education and counselling
- Safety and independence measures and home care needs
- Pain management
- Stress management and emotional support
- Nutritional counselling
- Vocational counselling
Correcting the symptoms of Depression during Neurorehabilitation significantly improves outcomes.